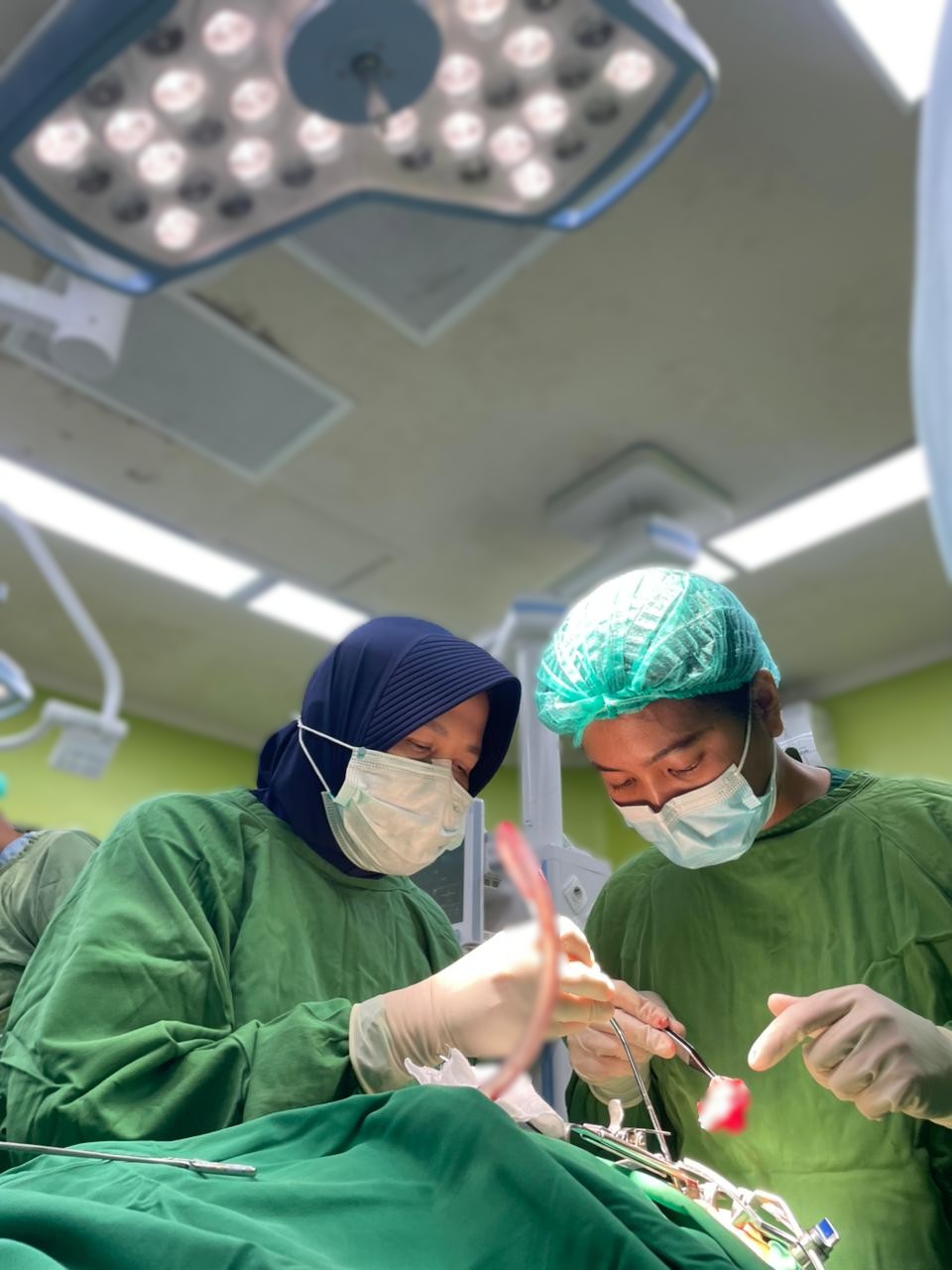
Not all children begin life under the same conditions. Some are born with clefts in their lips or palates. But in a regional hospital in East Lombok earlier this February, a group of children gradually rediscovered something simple yet fundamental—a blooming smile.
For several days, the operating room at RSUD dr. R. Soedjono in Selong, East Lombok, West Nusa Tenggara, witnessed the meeting of limitations and hope. Sixteen patients—mostly infants and toddlers—underwent free cleft lip and palate surgeries from February 5–8, 2026. The initiative was a collaboration between RSUD dr. R. Soedjono, Smile Train, Yayasan Senyum Harapan Nusantara, and the Oral and Maxillofacial Surgery Program of the Faculty of Dentistry, Universitas Gadjah Mada (FKG UGM). The team included faculty members, residents, and alumni working together in a community service mission to restore smiles to 16 patients in Selong. For families, the medical procedures were not merely surgical interventions—they nurtured hope that their children’s smiles could greet the world again.
Limited Access to Healthcare
Cleft lip and palate are congenital conditions still found across various regions of Indonesia, particularly in areas with limited access to specialist services. Without treatment, these conditions can affect eating ability, speech, and psychosocial development.
In East Lombok, distance, cost, and limited facilities often hinder families from accessing advanced surgical care. The presence of a cross-institutional medical team thus became more than a social service program—it became a bridge between need and care.
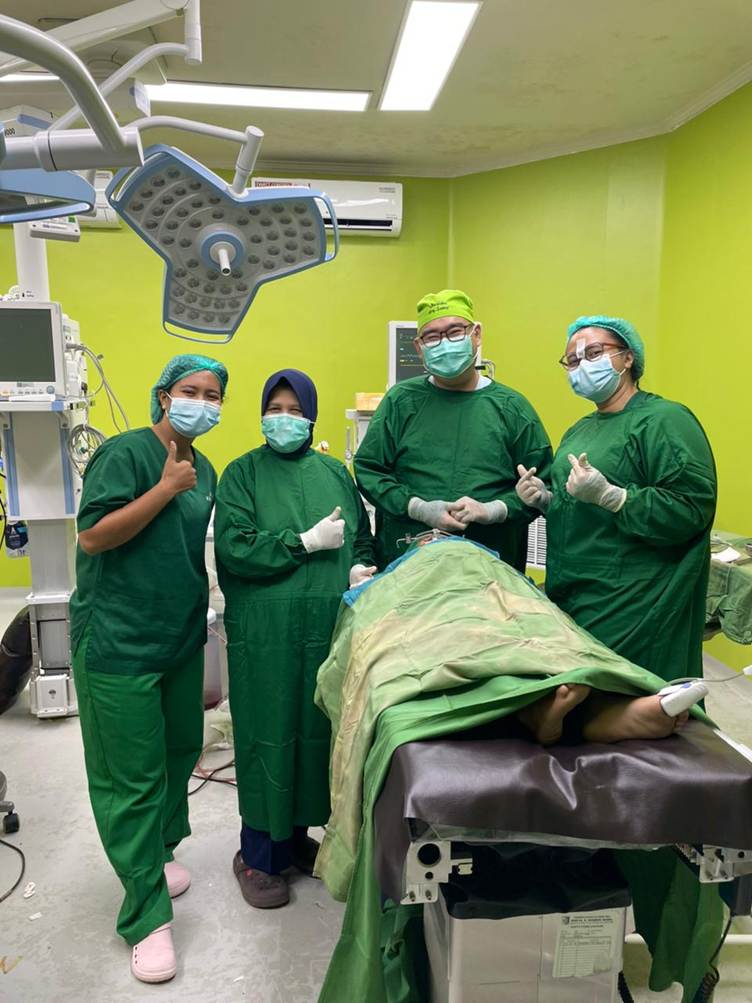
Silent Work Behind the Operating Table
Activities began with medical screenings on Thursday (February 5, 2026). Each patient underwent comprehensive evaluation to ensure surgical readiness, especially infants only a few months old. The team then determined the most appropriate surgical technique based on anatomical conditions and patient history.
Surgeries were performed throughout Friday (February 6, 2026), from morning until night. Techniques included Millard, Tennison-Randall, and Barsky labioplasty, as well as two-flap and Furlow palatoplasty. All procedures followed the principle of patient-centered care, placing patient safety and needs at the core of medical decisions. Despite the long schedule, the team conducted postoperative visits to ensure safe early recovery.

Learning, Sharing, and Maintaining Quality
The activity also served as an important clinical learning opportunity. Faculty members, residents, and alumni of the Oral and Maxillofacial Surgery program worked side by side, discussing cases and sharing field experiences. Collaboration with the regional hospital strengthened service networks and enhanced healthcare human resource capacity. This approach reflects a long-term effort—not merely resolving today’s cases, but building a stronger system for the future.
Health Education
Surgery is not the end of the journey. On Saturday (February 7, 2026), the team conducted health education sessions for families, discussing postoperative care, the importance of continued follow-ups, and nutritional and psychosocial support.
For parents, this knowledge serves as preparation for their children’s future. In a recovery room, a mother held her sleeping baby, delicate stitches visible on the infant’s lip. “The important thing is that later he can eat and speak well,” she said softly.

Keeping Hope Alive
Behind statistics and activity reports, this social service reminds us that healthcare access remains unequal. For some communities, a child’s smile does not come easily.
In Selong, East Lombok, those smiles are returning—slowly, one by one. From Selong grows the hope that no matter how wide the cleft, it can be united when compassion and expertise work together to find the way forward.
(Editor: Andri Wicaksono, Photo: Archive of the Oral & Maxillofacial Surgery Department, FKG UGM)