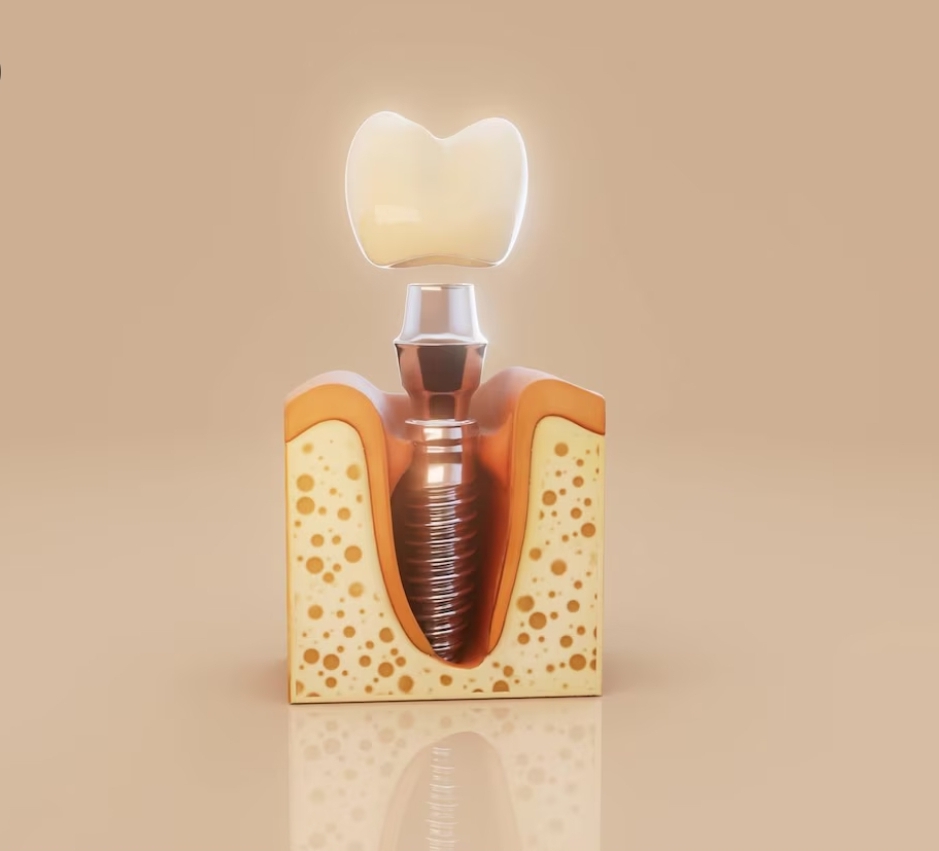
Titanium and its alloys have long been the backbone of dental implantology due to their combination of mechanical strength, light weight, corrosion resistance, and biocompatibility. However, as an inert material, titanium has limitations in terms of osseointegration and additional biological activities such as antimicrobial effects or advanced cellular interactions. Therefore, extensive research has focused on surface modification or the application of additional biomaterial coatings so that titanium implants are not only mechanically stable but also more biologically “active.”
One notable modification is aluminum oxide (Al₂O₃) coating using sputtering techniques combined with acid etching, as studied by Adella Syvia Maharani under the supervision of drg. Murti Indrastuti, M.Kes., Sp.Pros(K) and Dr. drg. Suparyono Saleh, Sp.Pros(K) in the study titled “Pengaruh Lama Etsa Asam pada Implan Gigi Titanium dengan Pelapisan Alumunium Oksida (Al2o3) Metode Sputtering terhadap Persentase Hemolisis (Kajian In Vitro).” This research examined hemolysis (blood cell response) to assess the safety of titanium surface modifications.
Research Focus: Acid Etching Duration, Al₂O₃ Coating, and Hemolysis
In the study, titanium implants were coated with Al₂O₃ using the sputtering method. The surfaces were then subjected to acid etching for varying durations to modify surface topography or roughness. The primary objective was to evaluate how long acid etching could be applied without significantly increasing hemolysis (red blood cell damage), as excessively rough or reactive surfaces may damage blood cells during initial contact or implantation.
These findings underscore the importance of balancing enhanced osseointegration with hemocompatibility (blood compatibility) in biomaterial surface design.
Strategies for Biomaterial Innovation in Titanium Implants
Several modification and innovation approaches are currently developing in the field of titanium implants:
- Bioactive Coatings
- Bioactive glass, hydroxyapatite (HA), or calcium silicate glass coatings can stimulate bone formation at the implant interface.
- Techniques such as magnetron sputtering, electrophoretic deposition, and dip-coating are commonly used.
- Chemical Surface Modification / Ion Implantation
- Doping titanium with ions such as calcium (Ca) or silicon (Si) via ion implantation or ECRIS can enhance bioactivity and reduce hemolysis.
- Nano–micro surface structures can improve osteoblast response and strengthen bone bonding.
- Al₂O₃ / Ceramic / Metal–Oxide Composite Coatings
- Al₂O₃ or ceramic film coatings can create favorable surface roughness and hardness.
- Coatings combined with materials such as TiB₂ have been reported to improve corrosion resistance, biocompatibility, and wear resistance.
- Antibacterial Surface Design / Antimicrobial Ions
- Titanium implants incorporating antibacterial elements such as copper (Cu) or other metal ions have been studied to suppress biofilm formation and peri-implant infections.
- Controlled ion release can inhibit bacterial colonization while remaining safe for bone tissue.
- Laser Techniques / Micro–Nano Texturing
- Ultrafast pulsed laser (femtosecond) techniques or micro–nano texturing can create surface patterns that favor cellular response and bacterial resistance.
- Micro–nano rough surfaces can enhance wettability and facilitate protein diffusion that supports osseointegration.
Challenges and Considerations
- Hemocompatibility
Surface modifications must be tested to ensure they do not increase hemolysis, especially during initial blood contact. - Balance Between Roughness and Surface Integrity
Excessive roughness may cause mechanical stress or microcracks, while overly smooth surfaces may reduce bone adhesion. - Coating Stability and Delamination
Coatings must withstand oral conditions (corrosion, cyclic loading) without peeling or degradation. - Ion Dosage and Controlled Release
Antimicrobial ions must be released at safe, non-toxic yet effective levels. - Long-Term Clinical Validation
Many studies remain at the in vitro or animal stage; long-term human clinical trials are required.
***
Titanium-based biomaterial innovations for dental implants continue to evolve, from surface modifications to functional active coatings. Research examining treatments such as acid etching on Al₂O₃-coated titanium implants with hemolysis measurements demonstrates that biological safety must not be overlooked in implant surface design. The combination of bioactive coatings, ion doping, micro–nano texturing, and antimicrobial elements offers promising opportunities for the development of biologically smarter and more functional titanium dental implants.
References
Adella Syvia Maharani, drg. Murti Indrastuti, M.Kes., Sp.Pros(K) ; Dr. drg. Suparyono Saleh, Sp.Pros(K), Pengaruh Lama Etsa Asam pada Implan Gigi Titanium dengan Pelapisan Alumunium Oksida (Al2o3) Metode Sputtering terhadap Persentase Hemolisis (Kajian In Vitro), https://etd.repository.ugm.ac.id/penelitian/detail/226609
Author: Rizky B. Hendrawan | Photo: Freepik