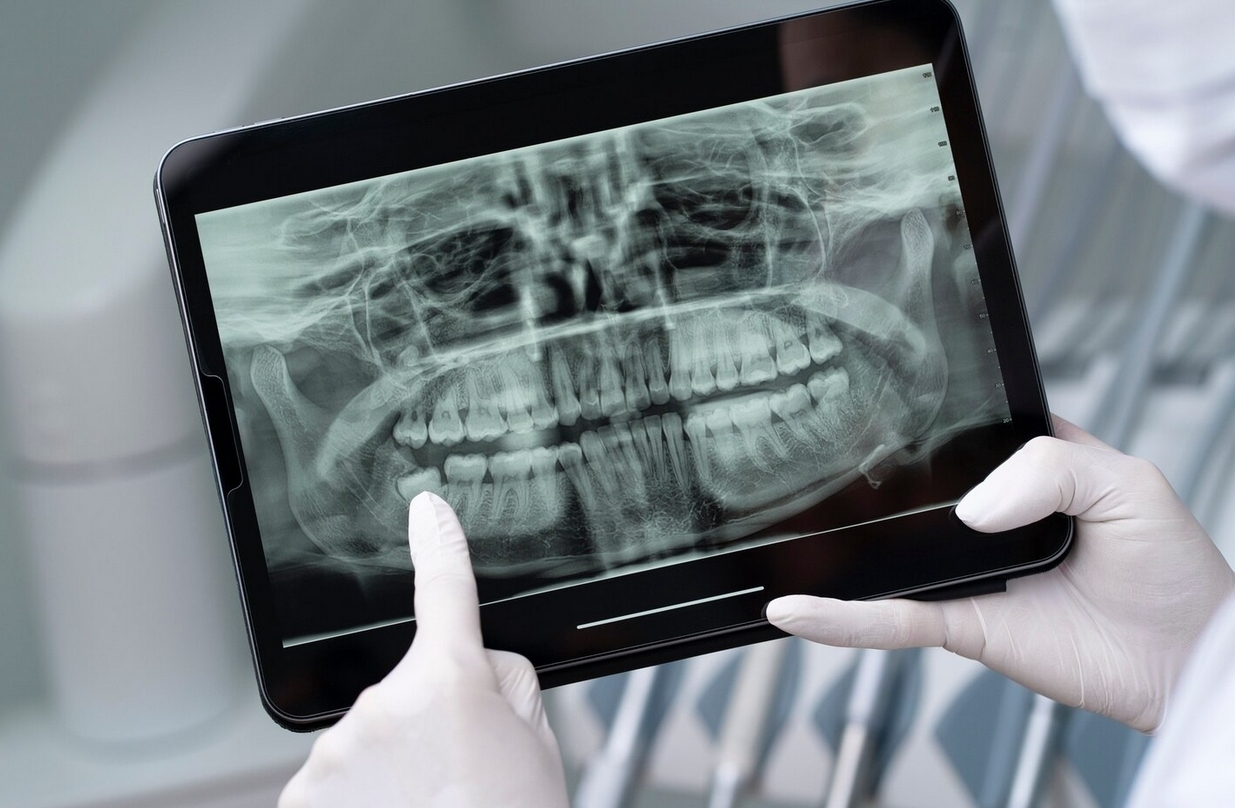
Radiology is an integral part of modern dental practice, playing a crucial role in diagnosis, treatment planning, and evaluation of therapeutic outcomes. Although radiography offers substantial benefits, exposure to ionizing radiation carries biological risks if not properly controlled. Therefore, radiation dose optimization is a fundamental principle to ensure that diagnostic benefits always outweigh potential risks.
Optimization means obtaining the best possible image quality with the lowest reasonable radiation dose, in accordance with the international ALARA principle (As Low As Reasonably Achievable).
Challenges in the Use of Radiation in Dentistry
In clinical practice, various radiographic techniques are used, including intraoral radiography, panoramic imaging, and cone beam computed tomography (CBCT). Each modality has different dose characteristics and clinical purposes:
- Intraoral radiography is used for detecting caries, periapical pathology, and evaluating restorations.
- Panoramic radiography provides a comprehensive view of the jaws and surrounding structures.
- CBCT offers high-resolution three-dimensional information for complex analyses such as implant planning and jaw bone abnormalities.
These technological differences directly affect the radiation dose received by patients. Therefore, dose control and optimization are essential to ensure patient safety without compromising diagnostic quality.
Related Research
A study conducted by FKG UGM student Lia Rahmawati under the supervision of Dr. drg. Rurie Ratna Shantiningsih, MDSc., and drg. Ryna Dwi Yanuaryska, Ph.D., titled “Differences in Radiation Dose in Intraoral, Panoramic, and Cone Beam Computed Tomography Using Thermoluminescent Dosimeters”, showed significant variations in radiation dose depending on the type of examination.
The results revealed that CBCT produced the highest dose, followed by panoramic and intraoral radiography. These findings highlight the importance of selecting the appropriate imaging modality according to clinical needs and implementing dose optimization strategies, especially in patients requiring repeated examinations.
Radiation Dose Optimization Strategies
Several approaches can be applied to optimize dose in dental radiology, including:
- Appropriate Selection of Radiographic Technique
Each clinical indication should be matched with the modality that provides sufficient information at the lowest dose. For example, CBCT should be used only when three-dimensional information is truly necessary. - Use of Digital Sensors
Digital radiography requires lower radiation doses than conventional film-based systems. In addition, digital images can be enhanced without the need for repeat exposures. - Adjustment of Exposure Parameters
The use of exposure parameters such as kVp, mA, and exposure time should be tailored to the patient’s size and age. Proper adjustment can reduce dose without compromising diagnostic detail. - Radiation Protection and Equipment Calibration
The use of lead aprons, thyroid collars, and regular equipment calibration ensures that radiation emission remains within safe limits. - Operator Training and Awareness
Dental professionals must be knowledgeable about radiation protection techniques, efficient image interpretation, and dose limits recommended by organizations such as the ICRP (International Commission on Radiological Protection).
Clinical Benefits of Dose Optimization
Dose optimization not only protects patients from cumulative radiation effects but also provides additional benefits:
- Reduces the need for repeat examinations due to poor image quality.
- Improves efficiency of radiology services.
- Ensures occupational safety standards for healthcare workers.
- Builds public trust in the safety of radiographic services.
***
Radiation dose optimization is a crucial component of dental radiology practice. Research on dose differences between intraoral, panoramic, and CBCT imaging confirms that CBCT delivers the highest dose and should therefore be used selectively and based on clear clinical indications.
Through the adoption of digital technology, routine equipment calibration, and increased operator awareness, the ALARA principle can be consistently applied to deliver safe, efficient, and sustainable radiology services in line with the SDGs related to health and innovation.
References
LIA RAHMAWATI, Dr. drg. Rurie Ratna Shantiningsih, MDSc.; drg. Ryna Dwi Yanuaryska, Ph.D., PERBEDAAN DOSIS RADIASI PADA RADIOGRAFI INTRAORAL, PANORAMIK, DAN CONE BEAM COMPUTED TOMOGRAPHY MENGGUNAKAN THERMOLUMINESCENT DOSIMETER, https://etd.repository.ugm.ac.id/penelitian/detail/221280
Author: Rizky B. Hendrawan | Photo: Freepik