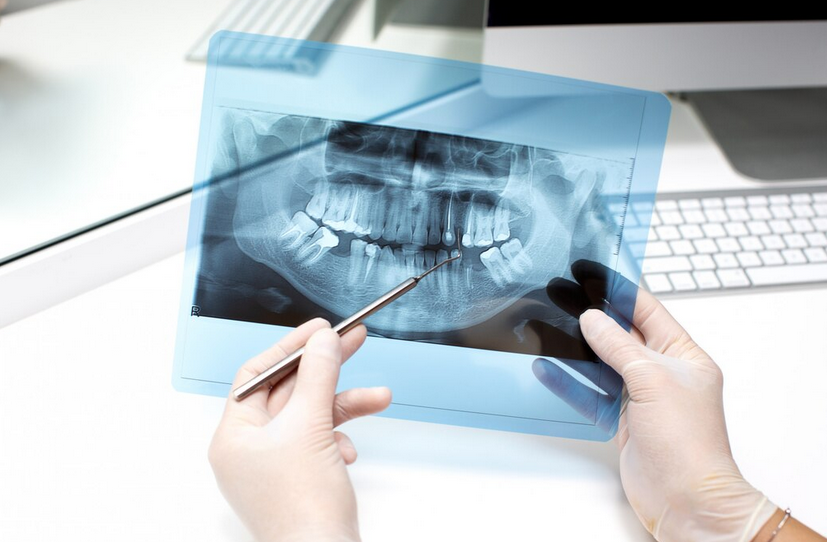
Oral malignant disorders—such as oral cancer—are frequently diagnosed at a late stage. These lesions tend to be locally invasive, have a high propensity for spread to cervical lymph nodes, and may metastasize to distant organs, resulting in decreased survival rates when diagnosis and treatment are delayed. Dentomaxillofacial radiology plays a vital role in early detection, staging, and treatment planning.
Commonly used imaging modalities include conventional radiography, Cone Beam Computed Tomography (CBCT), Computed Tomography (CT), Magnetic Resonance Imaging (MRI), and ultrasonography (USG). The choice of modality depends on the patient’s clinical condition, equipment availability, cost considerations, and diagnostic effectiveness.
Research Reference
Based on an article published in the MKGI Journal, Faculty of Dentistry, Universitas Gadjah Mada, authored by Dr. drg. Rini Widyaningrum, M.Biotech., Arif Faisal, Prof. Dr. Mitrayana, S.Si., M.Si., Prof. Dr. drg. Munakhir Mudjosemedi, S.U., and Prof. Dr. drg. Dewi Agustina, MD.Sc., MD.Sc., the authors emphasize that oral cancer is often detected at an advanced stage and that radiology using multiple techniques is essential for diagnosis, including three-dimensional and soft-tissue imaging modalities. “Oral cancer is a malignant neoplasia on the lip and oral cavity. It is generally late-detected, locally invasive, and it has a high propensity for cervical lymph node metastases as well as blood-borne distant metastases. Diagnostic imaging for oral cancer is generally performed using conventional radiography, Cone Beam Computed Tomography (CBCT), Computed Tomography (CT), ultrasonography (USG), Magnetic Resonance Imaging (MRI), Positron Emission Tomography (PET), Single-Photon Emission Computed Tomography (SPECT), and bone scintigraphy.”
Radiologic Modalities and Early Detection
Following are the main advantages and limitations of each modality in the context of early detection of oral malignant disorders:
| Modality | Advantages | Limitations |
|---|---|---|
| Conventional Radiography (intraoral, panoramic) | Low cost, widely available, capable of identifying bone changes, calcified lesions, and osseous destruction when infiltration occurs; suitable for initial screening in dental clinics. | Limited soft-tissue visualization, structural overlap, low sensitivity for small lesions or those not involving bone, and inability to detect soft-tissue invasion or lymph node metastases. |
| CT / CBCT | CBCT provides excellent visualization of hard tissue anatomy, jawbone invasion, and cortical perforation. Contrast-enhanced CT can demonstrate both hard tissue and certain soft-tissue involvement, supporting staging and surgical planning. | CBCT has limited soft-tissue resolution; higher radiation exposure compared to conventional radiography; cost and equipment availability may be limiting; metal artifacts may interfere with interpretation. |
| MRI | Superior soft-tissue visualization, including mucosal lesions, soft-tissue infiltration, edema, and tumor vascularity, without ionizing radiation. | High cost, longer examination time, contraindications in certain patients (e.g., metal implants), and in some cases lower sensitivity for small lesions compared to contrast-enhanced CT. |
| USG / Ultrasonografi | Useful for evaluating cervical lymph nodes and superficial soft-tissue tumors; relatively low cost; no ionizing radiation; suitable as a triage or complementary modality. | Limited usefulness for deep intraoral lesions; operator-dependent; lower resolution compared to CT/MRI; restricted penetration in complex anatomical regions. |
Diagnosis, Staging, and Treatment Planning
- Radiology is essential not only for tumor detection but also for staging, including assessment of tumor extent, soft-tissue and bone invasion, and lymph node involvement. Early detection significantly improves treatment success and survival rates.
- Modality selection should be individualized: suspected bone invasion favors CBCT or CT, while prominent soft-tissue symptoms such as swelling or ulceration may benefit from MRI or USG.
- Accurate interpretation requires strong knowledge of imaging principles, including density, contrast, windowing, use of contrast agents (CT/MRI), artifact recognition, and differentiation between normal and pathological anatomy.
Implications for Clinical Practice in Indonesia
- Many oral cancer cases in Indonesia are diagnosed late, partly due to limited access to advanced imaging modalities.
- Dentists must understand various imaging techniques and be able to interpret radiographs or CBCT images to recognize early signs such as cortical bone destruction, localized radiolucency or radiopacity, ill-defined lesion margins, or mucosal ulceration associated with trabecular changes.
- Public awareness and education should be strengthened to encourage earlier suspicion and referral for imaging evaluation.
***
Each imaging modality has specific strengths and limitations; an appropriate combination based on clinical context can improve diagnostic accuracy and therapeutic effectiveness. Strengthening image interpretation skills and expanding access to modern modalities such as CBCT, MRI, and USG are crucial steps toward improving early detection and increasing survival rates of oral cancer patients in Indonesia.
References
MKGI, Dr. drg.Rini Widyaningrum,M.Biotech., Arif Faisal, Prof. Dr. Mitrayana, S.Si., M.Si., Prof. Dr. drg. Munakhir Mudjosemedi, S.U., Prof. Dr. drg. Dewi Agustina, MD.Sc., MD.Sc., Oral cancer imaging: the principles of interpretation on dental radiograph, CT, CBCT, MRI, and USG, https://jurnal.ugm.ac.id/mkgi/article/view/22050
Author: Rizky B. Hendrawan | Photo: Freepik